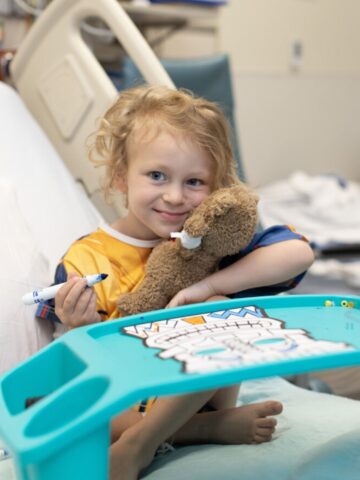
Among the many items decorating the walls and shelves of pediatric gastroenterologist Dr. Mitchell Katz’ office is a plaque given to him by a grateful family 10 years ago.
A large spoon is mounted in the middle of it with the inscription:
Changing Lives One Bite at a Time.
Since April 2003, Dr. Katz and his multidisciplinary team in CHOC’s Intensive Inpatient Feeding Program (IIFP) have been doing just that.
The feeding clinic he and his team launched was a novel concept back then, and as it approaches its 20th anniversary in April 2023, it has attained international prominence.
“This has been, truly and honestly, the greatest joy of my professional career – and I say that definitively,” says Dr. Katz, the program’s director who has been at CHOC almost 30 years.
“We’ve changed lives,” he adds. “What we do isn’t sexy in the sense of heart or brain surgery, but we have changed the lives of some 350 children and their families in ways that are indescribably rewarding.”
Just ask Helen Ghaly, a 24-year-old recent college graduate who is married with a 5-month-old girl, Kathryn.
Kathryn, Helen is happy to note, eats like a champ.
The opposite was true for Helen, the first patient in the IIFP.
Born premature at 27 weeks, and weighing only 1 pound 3 ounces, Helen was on a gastrostomy tube (G-tube) through age 5.

Until they enrolled Helen in the IIFP, her parents had little hope that she would ever eat normally. Food made her vomit, forcing Helen to rely on a surgically placed device that pumped liquid nutrition directly into her stomach.
“It’s every parent’s inherent responsibility to feed their child,” Dr. Katz says, “and if they can’t do that and have to reach for a G-tube, they feel like a failure.”
A year in the works
The genesis of CHOC’s IIFP was a conversation Dr. Katz had in the neonatal intensive care unit (NICU) in 2002.
“I was sitting in the NICU and a speech therapist and occupational therapist came up to me and said, ‘We have an idea,’” Dr. Katz recalls. “’We put all these G-tubes in kids, but we feel there’s something we could be doing to help these kids get off their G-tubes down the line. What do you think about setting up some kind of program?’
“I told them, ‘OK!’”
The three then consulted a dietician, psychologist, social worker and a nurse practitioner. The group met every Tuesday morning before their regular shifts for about a year until “we felt brave enough to admit a patient,” Dr. Katz recalls.
That turned out to be Helen.
“At the time,” Dr. Katz recalls, “there wasn’t a lot in the literature about this kind of program. We set up initial goals and flew by the seat of our pants. We were successful, and nothing breeds success like success.”
A multidisciplinary team involved in the Intensive Inpatient Feeding Program
The key to the success of CHOC’s IIFP is its multidisciplinary approach and its strict regimen, program officials say. There’s a reason it’s called “intensive.” Patients spend 19 days in the hospital and the same parent must be with them the entire time.
Although up to 70 percent of patients are G-tube dependent because they were born premature or have other medical conditions, the rest, like Helen, don’t take to food at all or are very restrictive eaters. Helen simply couldn’t stand the texture of food, so she avoided it.
Other patients, say, only will take nutrition from a bottle while sitting on a couch and watching TV, while others only will eat three types of food such as crackers, chips, and nuts. This is known as disordered eating.
Inpatients in the IIFP can undergo exposure therapy, where CHOC specialists carefully introduce them to different foods. Some need to work on their eating mechanics, while others need to reach a comfort level with food.
Helen recalls being in a room with a dog that wouldn’t be able to eat until she did.
She also recalls making cookies with a clinician.
“I was very physically sensitive as a kid because of being born prematurely,” Helen says of her aversion to food.
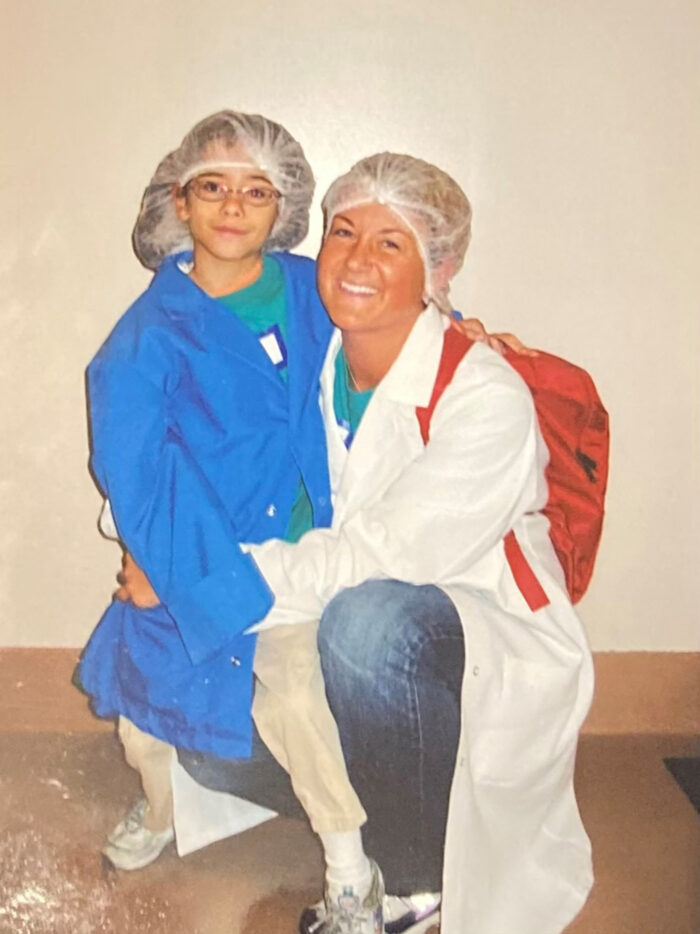
By the time her 19 days were over, Helen was off the G-tube.
“I remember the ‘pop’ sound it made when Dr. Katz took it out,” she says.
Imagine the frustration of Helen’s parents struggling to get her to eat several times a day with her twin brother, who had no issues with food.
Imagine Helen finally being able to eat as her brother and parents did.
“CHOC’s feeding program gave us hope that she would be able to eat normally one day,” says her mother, Helen Kraus. “Sure enough, it worked, and we’re forever grateful.”
Making a difference
Jazmine Bustos, NP, transferred to the IIFP from the pediatric intensive care unit (PICU) four years ago. The 11-year nursing veteran at CHOC didn’t know much about it when she applied.
“The first thing that caught my eye was the team aspect of the program,” Jazmine says. “During the interview process, I fell in love with this position. The PICU has a special place in my heart, but I felt I could really make a difference with these families.”
Jazmine says the team works seamlessly together and she feels her voice is respected.
“It’s amazing to see the effects of the work we do here,” says Jazmine, the mother of a healthy 2-year-old girl, Mia. “Most of the time, the families are emotional and so grateful for how much this means to their daily lives.
“I can only imagine the struggles these parents go through to meet the nutritional and weight goals of their child.”
CHOC finds success in feeding the ‘the toughest of the tough’
Dr. Katz says a seminal moment for the IIFP came in 2014 when his team published a paper of clinical results.
Key finding: 80 percent of inpatients were able to successfully get off their G-tube after their 19-day stay.
“We really became known on the landscape of feeding,” Dr. Katz says.
He adds: “If we’re 100-percent successful, we’re not getting the right kids. We get the toughest of the tough, and that’s who we want.”
Dr. Katz often is invited to speak at national research consortiums. In mid-July, he went to Baltimore to attend an event held by a society he helped set up, the International Association of Pediatric Feeding and Swallowing (IAPFS).
Success stories like Helen’s continue to seal CHOC’s stature in the field.
“The feeding program really changed my life,” says Helen, who now loves to cook. Her favorites include chicken, seafood and vegetables. “I want other kids and their families who are in a similar situation I was in to know that they are awesome and the program is awesome.”
Waiting to put on the crown
Another item in Dr. Katz’ office, located on the second floor of the CHOC West building, is an emperor’s crown costume hat still wrapped in plastic.
He won’t put it on, he says, until his vision for the feeding program, outlined in a proposal in May 2017, becomes a reality.
CHOC, he says, has the potential to become the first pediatric hospital to have a comprehensive feeding program under one roof for all of the hospital’s service lines, offering both inpatient and outpatient services.
By bringing together multiple treatment modalities in an innovative, collaborative fashion, the proposed Institute for Nutritional Intervention & Wellness will identify and treat patients and transform lives, and secure CHOC’s position as the leader in the treatment of disordered eating, Dr. Katz says.
“Nothing like this exists in the country and this could become a hallmark program at CHOC,” he says.
And if it happens, Dr. Katz will proudly put on his crown.
Learn more about CHOC’s Multidisciplinary Feeding Program