A study co-lead by Dr. Jennifer Gelinas, a pediatric neurologist at Rady Children’s Health Orange County and an associate professor in the departments of Pediatrics and Anatomy & Neurobiology at UC Irvine, has been recognized as one of the top 10 brain research advances of 2025 by the National Institute of Neurologic Disorders and Stroke (NINDS).
Dr. Gelinas, whom her colleagues at the hospital formerly called CHOC hail as a gifted physician scientist, was honored, along with a team of collaborators, for animal-based research that soon may help preserve brain function in pediatric patients with epilepsy.
The NINDS’ designation, announced in March 2026, characterized the study by Dr. Gelinas and her team as some of the finest in the neuroscience research community.
Dr. Gelinas was co-lead primary investigator of the study, “Closed-loop electrical stimulation prevents focal epilepsy progression and long-term memory impairment.” Her co-lead PI was Dr. Dion Khodagholy, a Henry Samueli faculty excellence professor of Electrical Engineering and Computer Science at the UCI Samueli School of Engineering.
“It’s an honor, and it was unexpected,” says Dr. Gelinas, whose study, published in Nature Neuroscience, began a few years before she joined Rady Children’s Health in July 2024 at Columbia University, where she served as an assistant professor of neurology and where she worked with Dr. Khodagholy and their collaborative lab groups.
“We were, of course, highly motivated to work this project because we think it does have potential translational impact,” adds Dr. Gelinas, who holds both medical and doctoral degrees from the University of Alberta. “It’s really exciting for work in this area to be recognized.”

Potential new treatment option
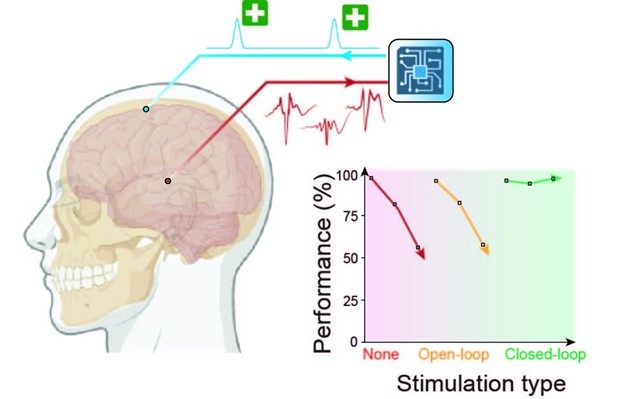
Dr. Gelinas and her team created a protocol assessed in rats with epilepsy that involved the use of adaptive, or closed-loop, brain stimulation. Also called neuromodulation, this therapeutic technique uses real-time feedback to adjust electrical stimulation based on monitored physiological signals.
The study findings identify a potential new treatment option for preventing epilepsy progression and preserving long-term memory in humans.
Abnormal brain activity patterns associated with epilepsy can negatively impact ongoing brain functions, including memory, communication, and learning. Current epilepsy treatments primarily aim to control seizures, and there are no directed treatments for these types of associated cognitive dysfunction.
The researchers set out to explore why some patients experience progressive worsening of their epilepsy and cognitive dysfunction and how to address it. They focused on interictal epileptiform discharges (IEDs), which are a ubiquitous pathologic finding in the brain signals of patients with epilepsy.
“We found that IEDs generate abnormal brain activity in other connected brain regions,” Dr. Gelinas explains.
This abnormal coupling of activity between different regions of the brain expands the ability to produce IEDs and is associated with the progression of epilepsy. Furthermore, this coupling of activity impairs long-term memory in an animal model of epilepsy.
“We designed a closed-loop electrical stimulation protocol to eliminate this abnormal coupling,” says Gelinas, “and were able to prevent the spread of the epileptic network and preserve the long-term memory of the animals despite ongoing seizures.”
Research inspired by patients
Dr. Gelinas’ study suggests that IEDs could be an important target for addressing both issues.
Dr. Gelinas says the study was inspired by clinical experience she’s had with children whose epilepsy has been difficult to treat, a situation in which concerns about long-term neurodevelopmental and cognitive outcomes are high.
“We started out trying to understand specific mechanisms in the brain that contribute to this cognitive dysfunction, because if we can identify a biomarker, there could be the opportunity to intervene in real-time,” Dr. Gelinas explains.
The research team implanted electrodes into the brains of freely moving rats who were developing epilepsy and who showed cognitive impairments on memory tasks.
“We figured out that there is a particular pattern of brain signals that are basically being transmitted from one region of the brain — the hippocampus — to another — the cortex — and that strongly seems to correlate with cognitive impairment,” Dr. Gelinas explains. “The concept is that the epileptic activity is getting in the way of the physiologic communication that we typically need for memory.”
The closed-loop electrical stimulation protocol that detects normal epileptic activity is not seizure activity but rather interictal activity, such as spikes, sharp waves, or high-frequency oscillations that occur between seizures in patients with epilepsy.
“These very brief bursts of abnormal activity were detected in real time, and we figured out what electrical stimulation we could administer to the cortex to prevent those IEDs from transmitting nonsense information and overriding physiological content required for memory,” Dr. Gelinas explains.
Next steps
Dr. Gelinas and her research colleagues performed analytical work that concluded that similar types of brain patterns are present in human patients with epilepsy.
The team now is trying to figure out ways to safely test the same protocol in patients who already have invasive electrodes implanted for clinical reasons.
“This is hopefully going to be the basis of the next step, which is the translational piece of this work,” Dr. Gelinas says.
The team is in the process of obtaining regulatory approval to start to recruit Rady Children’s Health patients to undergo a brief testing phase of this novel stimulation protocol while the patients are in the hospital to see if it yields any benefits.
A culture of innovative research
Dr. Gelinas says one of the main reasons she and Dr. Khodagholy came to Rady Children’s Health/UCI was because of the translational opportunities here.
She said she had “enthusiastic encouragement” from Dr. Terence Sanger, chief scientific officer at Rady Children’s Health Orange County, and others about the interest and appetite for engaging in cutting-edge electrophysiology and neuromodulation.
“This is very unique in pediatric patients both nationally and internationally,” Dr. Gelinas says. “We were really excited by the team and opportunities here to really try and advance the work we’re doing to bring benefit pediatric patients.”

CHOC Hospital was named one of the nation’s best children’s hospitals by U.S. News & World Report in its 2025-26 Best Children’s Hospitals rankings and ranked in the neurology/neurosurgery specialty.