Dr. Ashish Chogle is more of a doer than a talker.
“I love that I get to explore solutions to problems and make the solutions into a reality,” says Dr. Chogle, medical director of pediatric gastroenterology. “CHOC has created an amazing environment of innovation.”
A concrete sign of this innovation is the host of modules growing throughout the CHOC enterprise that use augmented reality (AR) or virtual reality (VR) technologies to enhance patient care.
CareXR, an app developed by Dr. Chogle and clinical nurse Wanda Rodriguez, in partnership with the Innovation Lab and BioFlight VR, was created to teach parents how to provide care at home for their children discharged with G-tubes, tracheotomies and central lines.
It provides immersive hands-on training for parents to practice skills prior to discharge, and offers an at home app-based version of the information to repeat post discharge.
CareXR is just one example of an AR/VR module in use or in development since the first, MRI with Choco, was launched two years ago.

“CHOC is going to great lengths to explore innovative ways to best support our patients and families,” says Debra Beauregard, who is part of part of the leadership team at the Sharon Disney Lund Medical Intelligence, Information, Investigation and Innovation Institute (Mi4), which creates, focuses and executes projects in the areas of medical intelligence and innovation in pediatric medicine.
“We’re collaborating all throughout the hospital to design a wide variety of solutions maximizing the benefits of augmented and virtual reality benefitting our patients and families.”
Partnerships
Working with outside partners such as Eon Reality, Bioflight VR, and Smiley Scope, CHOC aims to transform the patient experience through the use of AR/VR, which, along with artificial intelligence, is a main focus of pediatric cardiologist Dr. Anthony Chang, CHOC’s chief intelligence and innovation officer.
Augmented reality modules are ones in which users interact with computer-generated visuals and sounds in a real-world environment through mobile devices such as tablets and smartphones. Virtual reality completely immerses the user in a 3D-simulated world by using specialized headsets for an enhanced experience.
Creating these modules involves the engagement of clinical teams, soliciting feedback from patients and parents, and collaborating with a talented team of storyboard artists, programmers and animators.
Dr. Chogle says he’s encouraged to create solutions for everyday problems that he faces as a clinician.
“It makes my job very interesting and even more rewarding,” he says. “For future innovators, for every 10 to 20 ideas you have, there will be one idea that will be groundbreaking. So do not stop imagining and do not stop trying.”
Adds Debra: “We want to support and empower our medical staff and associates to be innovators.”
AR/VR modules meet specified needs across CHOC departments
CHOC at Mission
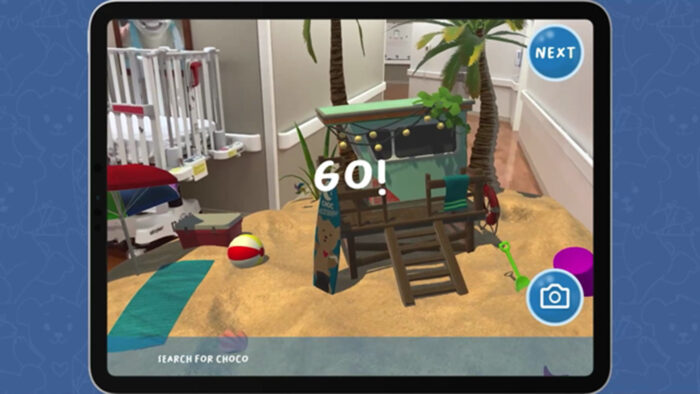
Choco’s Sea Adventure followed on the heels of MRI with Choco, which was designed to reduce anxiety about undergoing an MRI and was created in partnership with Mi4 and Eon Reality.
The AR experience takes patients on an exciting undersea adventure around the pediatric intensive care unit (PICU) at CHOC at Mission Hospital, transforming the hallways into a magical undersea adventure.
Choco’s Sea Adventure encourages patients who are recovering from surgery, injury or illness to get up and move, which helps in their recovery.
The team from CHOC Mission consisting of Melissa Kawanaka, child life specialist; Paula Moran, clinical nurse; Allison O’Berry, physical therapist; and Bronwyn Stackleather, director of patient care services; worked diligently with the Mi4 team and Eon Reality to create an innovative solution to encourage early mobility.
CHOC at Mission is also developing a module for patients with eating disorders that will help prepare them for admission to the medical stabilization unit. The team includes specialists from psychology, child life, clinical nutrition, and nursing.
“As with all of our modules, our patients and families are advising us every step of the way,” says Tiffani Ghere, part of the Mi4 leadership team. “We’re creating these modules for them, so it’s really important to include our families are part of our creative team.”
Cardiology
In response to the need for simple, accurate and accessible images for patient education, CHOC created a portfolio of AR heart modules. They include animated 3D versions of the normal heart as well as common conditions such as atrial septal defect (ASD), patent ductus arteriosus (PDA), and Coarctation of the Aorta (COA).
These modules can be used at the bedside to facilitate a discussion between patients and physicians and accessed at home by parents to review what was discussed.
“I think parents will really appreciate the ability to learn about their child’s condition and how we treat their child in this unique way,” says Dr. Gira Morchi, pediatric cardiologist and co-medical director of the CHOC Heart Institute. “It’s so different from the way we learned things when we were in medical school. To see this whole other side is fun and exciting.”
Designed with Eon developers and XR industry experts, cardiologists, such as Dr. Morchi, help write the script and record key education messages in the learning modules to help families understand the anatomy and physiology of the medical conditions.
“I enjoyed seeing how this was just the tip of the iceberg in applying new technologies and working with people who aren’t involved in practicing medicine, and how we were able to come together to apply our respective areas of expertise to create something to help our patients and families,” Dr. Morchi says.
Surgery center and OR
Dr. Zeev Kain, an international expert in the clinical management of perioperative fear and anxiety, participated in a module aimed at decreasing anxiety in patients scheduled for surgical procedures.
Patients are provided an iPad upon arrival at the surgical suite and can play games and use digital coloring books. The modules then take them all the way to the OR and up to the time when they fall asleep.

After learning about Dr. Morchi’s cardiac modules, pediatric surgeon Dr. David Gibbs, recently appointed assistant chief medical officer at CHOC, was inspired to help develop modules to educate parents in the different types of hernias and how they are repaired at CHOC.
“We’re starting with demonstrating how we repair four different types of hernias at CHOC,” Dr. Gibbs says. “Through improved education, we will reduce fear and anxiety for our families.”
During his lab years in the UC San Francisco Fetal Treatment Center, Dr. Gibbs had the chance to work in a hotbed of innovation.
“I thought that innovation was part of my past and not my future,” he says after coming to CHOC in 2001.
It wasn’t.
Over the years, Dr. Gibbs has become inspired to innovate as a way to improve patient care, such as by utilizing data to create predictive algorithms to improve care for trauma patients.
“My desire to be involved in innovation discovery has always been there,” Dr. Gibbs says, “but it’s been over the last few years that I’ve been able to put this into practice.”
In the future, Dr. Gibbs plans to create a module on pectus repair.
Oncology
Laps with Lois, named for one of CHOC’s resident dogs, will be a program aimed at improving the physical and psychological health outcomes of oncology patients.
This hybrid program will offer face-to-face interaction with Lois in addition to an AR version of her.
Lois and her handler, Child Life Specialist Chloe Krikac, will facilitate a walking intervention on the oncology unit to encourage physical activity and foster social connections.

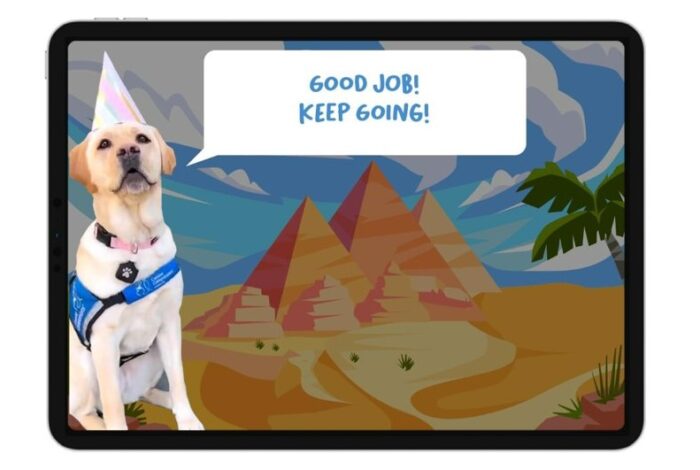
When Lois is not physically present, participants can interact virtually with the AR version of her on a tablet computer and engage in Laps with Lois on demand.
“We’re so excited for this project because it will benefit our kids, teens and young adults — not only physically, but emotionally as well,” Chloe says. “My hope for this project is to get teens and young adults out of their rooms more, socializing with their peers while engaging in physical activity.
“Our beloved Lois has a great ability to motivate people of all ages, and our hope is that this project will also help them connect with one another.”
Emergency Department
ED clinicians are currently working on a module to support children requiring stitches for lacerations. The goal is to decrease their anxiety about the procedure, while distracting them from the pain they experience, making the overall process easier for patients and families.
Waiting rooms in three specialties
CHOC cardiology, ophthalmology, and gastroenterology clinics are working on AR/VR modules with the aim to improve patient and parent satisfaction with wait times. These modules will provide both useful education as well as entertainment to families when they come for their specialty care visits.
Medical staff training
In addition to patient education and experiences, CHOC leaders are exploring ways to use AR and VR to create improved medical staff training methods. The virtual environments and 3D models augment learning with realistic health simulations, better visualization tools, and on-demand access for busy clinicians.
Just the beginning for innovative treatment and education strategies at CHOC
Championed by hospital leadership, physicians and providers, as well as Mi4, CHOC is pioneering the future of healthcare by developing and integrating advanced AR and VR technologies.
These innovative projects are enhancing patient and provider education, treatments and experiences, showcasing CHOC’s commitment to cutting-edge care.
Dr. Morchi says the word “innovator” was, at first, intimidating.
“I don’t think of myself as an innovator, and I imagine a lot of us do not,” she says. “But we are definitely problem solvers because that is what we must do daily. If one approaches innovation with the point of view that, ‘I have this problem that I want to solve’ and presents it to that team framed in that way, that can be the first step and things can move forward from there.
“We should think of innovation and the use of augmented reality as another tool in our tool kit of things we use every day to solve problems.”

Learn more about medical innovation at CHOC
The CHOC Sharon Disney Lund Medical Intelligence, Information, Investigation and Innovation Institute, known as Mi4, is the hub for innovation at CHOC. Mi4 accelerates innovation and insight that will advance the health and well-being of children.




