About a year ago, Grace Lozano, who has congenital heart disease (CHD) and Down syndrome, could barely sit still and focus for two minutes while being read to or working on a puzzle or engaging in other activities typical of a 5-year-old.
Now, her attention span has dramatically expanded to 15 to 20 minutes, and her parents, Desiree and Nick, are seeing improvements in other areas of concern, including hyperactivity and impulsivity.
What happened?
Although most people are not aware of the strong relationship between CHD and brain development, newborns with serious heart defects have a high risk of growing up with developmental delays, cognitive impairments, learning disorders, ADHD, autism, and emotional difficulties.

The positive changes in Grace, now 6, came after she underwent a thorough neuropsychological evaluation in October 2021 by members of the CHOC Heart Institute Cardiac Neurodevelopmental Clinic (CNC), who will present at an international conference this month about a highly successful new surveillance program of CHD patients.
Due to advances in surgical techniques and medical therapies over the past several decades, mortality rates for children and adolescents with complex CHD have significantly declined.
Thus, it has become critical to address cognitive, learning and behavioral concerns experienced by these patients as they age, says Dr. Alexander Tan, director of CHOC’s CNC, which accepts referrals for children with CHD 3 and older and continues care for surgical patients during early childhood.

Surveillance program launched for cardiac neurodevelopmental clinic
Although the American Heart Association and American Academy of Pediatrics published a landmark paper in 2012 recommending the need for periodic surveillance of CHD patients, differences in surveillance methods have resulted in significant variations in referral outcomes across cardiac neurodevelopmental programs in the U.S.
At the start of fiscal year 2022, CHOC implemented a formal surveillance program to assess referral and clinic outcomes for its CNC.
The program included development of a surveillance checklist to be administered by cardiologists during medical visits to systematically screen for neuropsychological concerns and family interest warranting referral for evaluation. Provider handouts and educational materials also were developed to improve family education.
Compared to fiscal year 2021, when no formal surveillance existed, the new program resulted in significant increases in referral (74.42%) and clinic volume (185.71% increase).
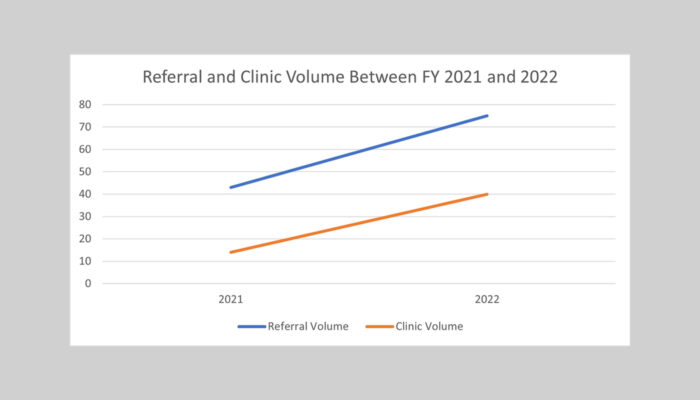
from FY 2021 to 2022
“We’ve made significant advancements, highlighting the importance of systematic monitoring and education on family awareness and motivation to participate,” says Dr. Tan, whose team will present its findings at the CNOC (Cardiac Neurodevelopmental Outcome Collaborative) conference in Montreal Oct. 25-27.
“We’re trying to figure out ways of doing things better, more efficiently, and more completely, and we wanted to share this information with other groups,” said pediatric cardiologist Dr. Wyman Lai, medical director of echocardiography at CHOC and former co-medical director of the CHOC Heart Institute, which collaborates closely with the CHOC Neuropsychology Program to better treat CHD patients as they transition from childhood to adolescence to adulthood.

CHOC amongst select company for CNOC
CHOC is among a few hospitals in California that are members of CNOC.
Prior to coming to CHOC in October 2020, Dr. Tan trained under one of CNOC’s top physicians and published a paper earlier this year on research he conducted while at Children’s Healthcare of Atlanta that examined adaptive functioning in adolescents with CHD who were referred for neurodevelopmental follow-up.
He also published a paper (“Implementing Standard Screening for Autism Spectrum Disorder in CHD”) in 2021 advocating for the implementation of autism screening in children with CHD to be a consistent standard of care.
In addition to Dr. Tan and Dr. Lai, Heather Hennrick, PhD, worked on the formal surveillance program project that will be presented in Montreal as a neuropsychology post-doctoral fellow at CHOC, along with nurse practitioner Elizabeth Miller, MSN, CPNP, and Marissa Olson, RN, a clinical nurse in CHOC’s cardiovascular ICU (CVICU).
“Awareness of the neurodevelopmental component of kids with CHD is still lacking,” Elizabeth says, “so the point of our surveillance project was to elicit a response from parents to think about their child in a neurodevelopmental way during their cardiology visits.
“It really was a big educational piece for CHOC’s entire cardiology community — parents included.”
CHD is a common developmental abnormality
CHD affects nearly 40,000 newborns each year, making it one of the most common developmental abnormalities.
Over 90 percent of children with CHD are expected to survive into adulthood. There are more than 1 million adults with CHD in the U.S.
Grace was born prematurely (35 weeks) with two large holes in her heart. She stayed in the neonatal intensive unit (NICU) for three weeks and went home with a gastrostomy tube (G-tube) since she had issues with taking in nutrition orally.
Thoracic surgeon Dr. Richard Gates, director of cardiothoracic surgery at the CHOC Heart Institute, repaired Grace’s heart defect when she was 5 months old.
Last year, Grace’s cardiologist, Dr. Pierangelo Renella, referred her to CHOC’s CNC and she saw Dr. Tan in October.
“We really wanted to understand what her weaknesses were as well as her strengths, and we wanted to advocate for Grace to have an equal opportunity at school,” Desiree says.


The brain and behavior
Dr. Tan, who has a Ph.D. in clinical psychology with a specialization in pediatric neuropsychology, performed a thorough neuropsychological evaluation of Grace, studying the relationship between her brain and her behavior.
The assessment included assessing Grace’s brain function and understanding her strengths and weaknesses and looking for such diagnoses as autism, ADHD, and learning disorders.
Dr. Tan diagnosed Grace with global developmental delay, an umbrella term used when children are significantly delayed in their cognitive and physical development, and recommended school and community services for her to access and a plan to monitor her development moving forward.
“He provided a detailed report on Grace including how schools should service her and what therapies they should be focusing on,” Desiree says. “I didn’t realize there was a doctor who could help us advocate for her, and now we have all this knowledge.”
Effective behavior analysis (ABA) therapy
Dr. Tan determined that Grace could learn a lot but that her behaviors were preventing her from doing so.
Due to the importance of early intervention, he recommended she begin applied behavior analysis (ABA) therapy and immediately connected her to Innovate ABA, a local outpatient clinic that he says provides quality ABA care.
ABA therapy uses individualized interventions and instructional strategies to improve functional skills and decrease disruptive behaviors. The practice is used most extensively in special education and the treatment of autism.
Desiree says ABA therapy worked great, helping to greatly expand Grace’s attention span and minimize some of her disruptive behaviors.
‘A blessing’
Grace, who has an older brother, Nico, 10, and older sister, Leah, 9, is scheduled to see Dr. Tan again in a year.
“The care we received at CHOC has been a blessing,” Desiree says. “I’m so grateful we live in an area where we have access to so many resources that will make it possible for Grace to thrive.”

Says Dr. Tan: “This surveillance program is just one example of how we continue to advance in supporting the families of children with CHD to be educated and invested in their neurodevelopmental outcomes. It is essential that we monitor their thinking, learning, and behavior to make sure they have all the supports they need so they can have the best possible future.”

CHOC and UCLA Health together have been ranked among the top children’s hospitals in the nation for Cardiology & Heart Surgery by U.S. News & World Report.