CHOC now offers responsive neurostimulation (RNS) for refractory epilepsy, in addition to the already thriving vagus nerve stimulator program. This newer therapeutic option offers potential relief for patients with seizures emanating from multiple locations in the brain, or when seizure onset overlaps with eloquent cortical areas providing essential function, like language.
RNS therapy involves implanting an RNS System into the brain during surgery. An RNS System is a small neurostimulator, similar to a pacemaker, that is placed within the skull and is connected to two wires that are placed on the surface of the brain, in the brain or a mixture of both. This surgery is minimally invasive and does not require any tissue removal.
Once implemented, the neurostimulator monitors and responds to brain waves to detect seizure activity. When this activity is detected, the stimulator sends a signal of electrical current to the brain to stop the seizure or possibly prevent the seizure. The RNS System wirelessly collects information from the neurostimulator and uploads it to a database where a provider can review a child’s seizure activity and progress.
RNS therapy shows promise in pediatrics
While RNS is currently only FDA approved for patients 18 years and older, CHOC can offer this to select patients and aims to expand access to this intervention for the pediatric epilepsy population through participation in a multicenter clinical trial. RNS has proven to be very successful in adults and shows exciting promise for pediatric patients.
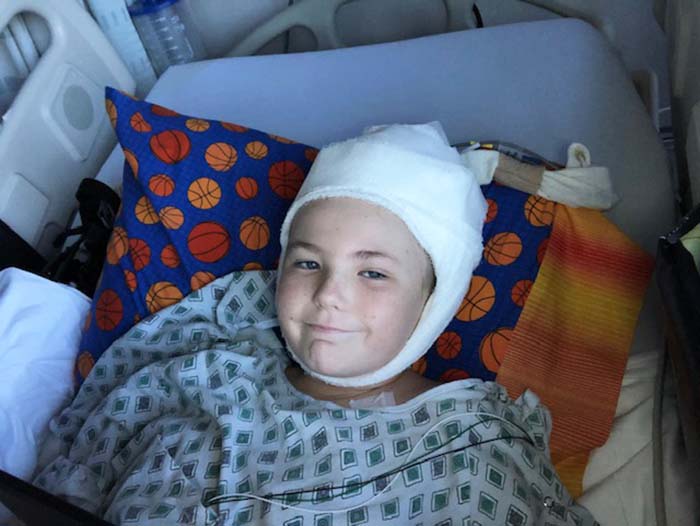
Typically, the candidates for this system have multiple areas of seizures or have seizures coming from an eloquent area, as did 11-year-old CHOC patient Bryce, who had a tumor growing near the motor cortex. Seven years prior, Bryce had undergone a complete tumor resection via craniotomy but started to experience breakthrough seizures due to the regrowth of the tumor.
During these breakthrough seizures, Bryce’s right arm would go completely numb for 30 seconds, and he would not be able to move it for a minute after. Occasionally the numbing sensation would even move down to his leg or affect his face. Nothing seemed to spark them, notes Jennifer, Bryce’s mom. These seizures could happen at any time and the frequency was always random.
To combat the seizures, Bryce had been through all the drug regimens currently available, and “the side effects were becoming intolerable. I just didn’t like putting more and more drugs into his body,” says Jennifer. They were searching for a more permanent solution that would allow this growing pre-teen to lead a more active life.
RNS surgery offers seizure control
Seizure and functional brain mapping confirmed that seizures were emanating from the cortex that controlled Bryce’s right hand. Historically, further treatment options sparing the motor cortex were unavailable.
However, partial resection of the tumor was performed and RNS electrodes were placed over the seizure onset zone, protecting the area controlling hand function. One-year post intervention, Bryce is nearly seizure-free. “I occasionally have a bit of tingling in my fingertips, but it doesn’t stop me from playing basketball,” he says. Jennifer quickly adds, “He is doing really well in school.”
The responsive nature of the RNS detects abnormal activity and reacts in real-time. Dr. Donald Phillips, Bryce’s epileptologist, can track seizures as they occur, and makes stimulation changes over time for even better seizure control. Dr. Phillips is delighted that his patient is nearly seizure-free, now one year post his RNS treatment. CHOC aims to expand access to the RNS treatment for the pediatric epilepsy population through participation in a multicenter clinical study. This treatment shows exciting promise to help more pediatric patients like Bryce.

CHOC Hospital was named one of the nation’s best children’s hospitals by U.S. News & World Report in its 2025-26 Best Children’s Hospitals rankings and ranked in the neurology/neurosurgery specialty.